Behind the brick walls of the Mycetoma Research Centre trying to unravel the mysteries of the infection is a rare story of medical success in impoverished Sudan.
With bandages on their swollen, deformed feet, patients from across the vast country arrive at the spotless facility set in a garden in the southern Khartoum district of Soba.
For more than 40 years, British-educated researcher Elsheikh Mahgoub has been searching for answers to the mysteries of mycetoma, a bacterial and fungal infection which can spread throughout the body resulting in gross deformity and even death.
Sudan is particularly affected by mycetoma, which is also endemic in a geographic belt including regional neighbours Chad, Niger, Nigeria, Ethiopia, Somalia, parts of Saudi Arabia and Yemen, experts say.
The belt also stretches to India and parts of Latin America.
Mycetoma is “a badly neglected disease”, the United Nations’ World Health Organisation (WHO) says on its website.
Yet in Sudan, researchers have been studying the condition since British colonial times, and the Khartoum centre has been globally recognised for its work.
Such acknowledgement in the health field is unusual for a country which ranks near the bottom of a UN human development index measuring income, health and education.
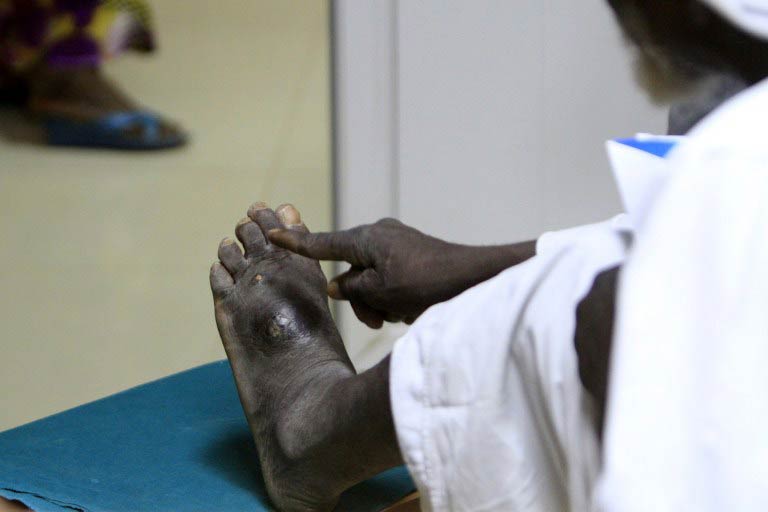
Mycetoma is characterised by swelling of the feet but it can eat away bone and spread throughout the body, causing grotesque barnacle-like growths, club-like hands and bulging eyes.
The traditional treatment was amputation – something the Sudanese centre tries to avoid.

“Most patients who get it are farmers, or animal herders, and these are poor people,” says Mahgoub (78).
“They are poor, and they get poorer.”
Mahgoub says he established Sudan’s first mycetoma centre in 1968, working with a British nurse and a British technician.
“Many people thought: Why should I be concerned about this disease which is not common, which is difficult to diagnose, and difficult to treat?” he told reporters on a tour of the facility, which opened at its current location in the 1990s.
The centre offers diagnosis, treatment, training and research as part of Soba University Hospital under the University of Khartoum, which funds it along with some donors.
It has its own laboratory, two wards, and is served by seven part-time doctors as well as Mahgoub, the research supervisor, and its director A.H. Fahal, a professor of surgery.
Though its resources are limited, they have been used effectively, Fahal has written.
Patients come and go – with 6 400 registered so far – but Fahal remains and so does Mahgoub, challenged by the puzzle of why mycetoma is so prevalent in Sudan and neighbouring countries.
“I think there’s two things,” Mahgoub explains, pointing first to the organism’s presence in soil.
He says people who make their living from the land are more likely to get pricked by thorns, for example, from the Acacia trees which are widespread in the mycetoma-prone region and provide a route for infection.
Secondly, the patients have been found with weakened immune systems. Some not only have mycetoma but also Aids, leprosy, tuberculosis or other conditions, Mahgoub says.
“Why? Why these people? Is it nutritional, because of malnutrition? Is it because of the other diseases they get at the same time?”
He does not yet have the answers.
“But we know that they have got some deficiency in their cell-mediated immunity.”
Thorn jab 20 years ago
Mohammed al-Amien Ahmad is a typical case.
The farmer tells Mahgoub that a thorn jabbed him about 20 years ago.
“This thorn came out and it seemed to be OK. Later on the swelling came up. It was a bit itchy,” says the goateed farmer, who is in his 60s and wears a traditional white jalabiya robe.
Ahmad, his enlarged left foot oozing pus, has travelled more than 500 kilometres by bus from Umm Rawaba where he farms about 70 acres of sorghum.
His condition worsened over the past two years, he says, forcing him to reduce the amount of land he can work, and cutting into his annual income of 30 000 – 40 000 Sudanese pounds ($4 300 – $5 700).
In a majority of cases mycetoma is painless, meaning patients like Ahmad delay seeking medical care.
This makes treatment more difficult, Mahgoub says.
“The main thing we tell them is to come early… Because if the swelling is small it can be excised in total,” with follow-up medication, he says.
The Mycetoma Research Centre provides diagnosis and any surgery patients may need for free. But patients may require months of anti-fungal medication, which they must buy themselves.
Some who cannot bear the financial burden stop taking their medicine, Mahgoub says.
“In that case the disease will just go back to where it started. That’s a real problem,” he says.
Drug prices in Sudan have climbed over the past two years as Sudan’s currency plunged in value and inflation soared.
Sudan’s health ministry has expressed concern about the emigration of doctors and other health professionals seeking better salaries and working conditions abroad.
Nationwide, there were 1.3 health workers per 1 000 people in 2011, against the WHO benchmark of 2.3.
Many primary health care facilities in Sudan “lack appropriate medical equipment and supplies, have inadequate infrastructure or are understaffed,” the United Nations said this year.
In contrast, the Mycetoma Research Centre “is recognised globally as a world leader”, an informal group of experts on the disease wrote after their first meeting this year in Geneva.
Ian Timberlake for AFP.